EMBRACE
Education and Mentoring to BRing Access to CarE for SCD
(EMBRACE)

To improve access to high-quality care for individuals living with sickle cell disease in the Southeast United States
The Education and Mentoring to BRing Access to CarE (EMBRACE) Network is a regional collaborative of 8 southeastern states (AL, FL, GA, KY, MS, NC, SC, TN) using collective impact strategies and continuous patient engagement to improve access to high-quality care for individuals living with sickle cell disease (SCD)
- Increase the number of providers adhering to NHLBI guidelines to provide care for persons with SCD
- Increase the pool of providers offering evidence-based SCD care by disseminating technology-based provider support tools (tele-mentoring and telemedicine)
- Develop and implement strategies to improve access to quality care in a SCD medical home with a focus on individual and family engagement.

EMBRACE Education | EMBRACE Engagement | EMBRACE Empowerment
In 2014 the National Heart, Lung, and Blood Institute (NHLBI) published Evidence-Based Management of Sickle Cell Disease: An Expert Panel Report. These guidelines were developed by an expert panel composed of health care professionals with expertise in family medicine, general internal medicine, adult and pediatric hematology, psychiatry, transfusion medicine, obstetrics and gynecology, emergency department nursing, and evidence-based medicine.
The Guidelines were created to:
- provide guidance for primary care physicians (PCP) on sickle cell management and care
- help sickle cell warriors receive appropriate care by providing the best science-based recommendations to guide practice decisions.
In an effort to ensure that sickle cell patient warriors are on equal footing with their provider and other stakeholders in the decision-making process, we’ve developed a new Expert Patient webinar series based on the NHLBI guidelines (EMBRACE Education).
Although immeasurably valuable, open patient/caregiver comments were not considered during the development of these guidelines. Consistent with the Consortium mission to ensure that the sickle cell patient/caregiver voice is at the center of everything that we do, we are hosting a series of focus groups to provide feedback on various aspects of the project, including opioid agreements, telemedicine, travel away from home, etc. (EMBRACE Engagement).
A diverse demographic of active, engaged focus group participants, will form state and regional Community Advisory Boards (CAB) to develop and execute action plans and strategies, necessary for the success of this project (EMBRACE Empowerment).
EMBRACE is all about the Warrior. Join the team!
Education and Mentoring to BRing Access to CarE (EMBRACE) Network
EMBRACE Education and become a patient expert.
Patient Education Webinars on Warrior University
The Sickle Cell Consortium has partnered with Atrium Health and the HRSA EMBRACE team, to launch EMBRACE Education, the first in a series of NHLBI-focused webinars, during the Summer 2019 semester of Warrior University.
The full NHLBI-focused program will serve to assist health care professionals in the management of common issues, including routine health maintenance, the recognition and treatment of common acute and chronic complications and comorbidities of SCD, as well as the indications for and monitoring of hydroxyurea and blood transfusion therapy.
HELP US TO IMPROVE CONTENT BY TAKING THE EMBRACE FEEDBACK SURVEY HERE
WATCH THE RECORDINGS:
- Blood Transfusions in Sickle Cell Disease: How, When, Why
- Blood Transfusions: Keeping It Safe – Blood Matching
- Diagnosis and treatment of acute chest syndrome
- Hydroxyurea in pediatric SCD
- Hydroxyurea for treatment of adult SCD
- Diagnosis and treatment of Avascular Necrosis
- Understanding the CBC: Part I – The Basics
- Keeping it Safe: Iron Overload
- Chronic pulmonary complications in people with SCD (pending)
- Stroke and other neurological complications in people with SCD (pending)
EMBRACE Full Playlist
Hydroxyurea & Sickle Cell Disease
Hydroxyurea for Children
Acute Chest Syndrome & Sickle Cell Disease
Understanding Your Complete Blood Count
Sickle Cell & Travel
EMBRACE Engagement
“Nothing for us, without us”
The EMBRACE Network (Education and Mentoring to Bring Access to Care), is a project that seeks to expand access to quality care, improve care delivery and provide knowledge and support.
Participate in a focus group.
Telemedicine, Travel Letter, Opioid Agreement, etc.
- Focus Group #1 – Travel
This first focus group will occur in-person at the 6th Annual Sickle Cell Patient & Family Educational Symposium. Visit www.sicklecellconvention.org to learn more.
- Focus Group #2 – The Opioid Contract
- Focus Group #3 – Telemedicine
- Focus Group #4 – Project ECHO
EMBRACE Empowerment
Join a State Community Advisory Committee.
COMING SOON.
EMBRACE a medical home
What is a medical home?
The Medical Home (also known as Patient or Family Centered Medical Home) is an approach to providing comprehensive primary care that facilitates partnerships between patients, clinicians, medical staff, and families.
Find a doctor near you
The purpose of these referrals are to help people with sickle cell disease identify a doctor with experience treating sickle cell warriors. The goal is to assure continued outpatient care for warriors so that we do not need to depend on emergency or hospital care.

EMBRACE | ECHO® | NHLBI Guidelines | CONTACT
Sickle cell is a genetic life-long disease characterized by episodes of severe pain, frequent hospitalizations, long-term organ damage and a shortened lifespan. Most physicians with expertise in sickle cell disease practice in academic healthcare centers or large medical centers. That means that there are large gaps in access to care. Lack of knowledge about the long-term effects of sickle cell disease and physician assumptions can lead to suboptimal care and a less desirable quality of life for these patients.
The EMBRACE Network (Education and Mentoring to Bring Access to Care), is a project that seeks to expand access to quality care, improve care delivery, and provide knowledge and support through regular ECHO® clinics, like virtual grand rounds, patient case presentations will be combined with didactic learning and mentoring. We invite you to participate in these sessions to engage with a team of multi-disciplinary specialists around the management of sickle cell disease.
ECHO® (Extension for Community Healthcare Outcomes), is an Internationally recognized tele-mentoring model that connects providers with specialists through regularly scheduled, interactive, tele-mentoring sessions.
Benefits of ECHO®
-
- Specialists train community providers in an area outside of their expertise
- Specialists use low-cost videoconferencing to conduct tele-ECHO clinics
- Expands access to care for rural and underserved patients
- Rapid dissemination of best practices
- Providers receive CME/CE and MOC II/IV points by participating in virtual grand rounds.
NHLBI GUIDELINES
Access the NHLBI Guidelines for Evidence-Based Management of Sickle Cell Disease.
The purpose of the “Evidence-Based Management of Sickle Cell Disease: Expert Panel Report (EPR), 2014” is to synthesize the available scientific evidence on sickle cell disease and offer guidance to busy primary care clinicians.
Readers should remember that the document is intended to provide guidance for management, not to be rigidly prescriptive.
Developed by an expert panel composed of healthcare professionals with expertise in family medicine, general internal medicine, adult and pediatric hematology, psychiatry, transfusion medicine, obstetrics and gynecology, emergency department nursing, and evidence-based medicine. Panel members were selected by the National Heart, Lung, and Blood Institute’s (NHLBI’s) leadership.
The purpose of these guidelines is to help people living with sickle cell disease (SCD) receive appropriate care by providing the best science-based recommendations to guide practice decisions. The target audience is primary care providers and other clinicians, nurses, and staff who provide emergency or continuity care to individuals with SCD. NHLBI sponsored the development of these guidelines to assist health care professionals in the management of common issues, including routine health maintenance, the recognition and treatment of common acute and chronic complications and comorbidities of SCD, as well as the indications for and monitoring of hydroxyurea and blood transfusion therapy. The guidelines address the care of infants, children, adolescents, and adults with SCD, with the goal of facilitating high-quality and appropriate care for all individuals with this disease.
CONTACT
For more information, contact Shirley Miller at (980) 442-2535 or Shirley.Miller@AtriumHealth.org.

The National Heart, Lung, and Blood Institute (NHLBI) published Evidence-Based Management guidelines in 2014 that focused on supporting primary care physicians to address challenges with access to quality. Dissemination and implementation of these guidelines remain suboptimal.
The Education and Mentoring to BRing Access to CarE (EMBRACE) Network is a regional collaborative of 8 southeastern states (AL, FL, GA, KY, MS, NC, SC, TN) committed to collectively engage with the SCD community and various stakeholders to:
- Increase the number of providers adhering to NHLBI guidelines to provide care for persons with SCD
- Increase the pool of providers offering evidence based SCD care by disseminating technology based provider support tools (tele-mentoring and telemedicine)
- Develop and implement strategies to improve access to quality care in a SCD medical home with a focus on individual and family engagement.
Education and Mentoring to BRing Access to CarE for SCD (EMBRACE)
Ifeyinwa (Ify) Osunkwo, MD, MPH
Ify.Osunkwo@carolinashealthcare.org
HRSA-17-078
Through regular ECHO® clinics, like virtual grand rounds, patient case presentations will be combined with didactic learning and mentoring. These sessions are open to health care providers who want to engage with a team of multi-disciplinary specialists around the management of sickle cell disease.
Benefits of ECHO®
-
- Specialists in sickle cell disease train community providers in an area outside of their expertise.
- Specialists use low-cost videoconferencing to conduct tele-ECHO clinics
- Expands access to care for rural and underserved patients
- Rapid dissemination of best practices
- Providers receive CME/CE and MOC III/IV points for participating.
Just as implementation of the NHLBI guidelines vary greatly among healthcare institutions, the uptake of guideline-recommended interventions remains low among sickle cell patient warriors*.
EMBRACE tackles this issue through Education, Engagement, and Empowerment.
|^ See EMBRACE Education, EMBRACE Engagement, EMBRACE Empowerment ^|
Principal Investigator(s): Osunkwo, Kanter, Strouse
Transition specialist(s): Coretta Jenerette
Community Engagement Partner(s): Sickle Cell Consortium
Healthcare Institution(s): Atrium Health
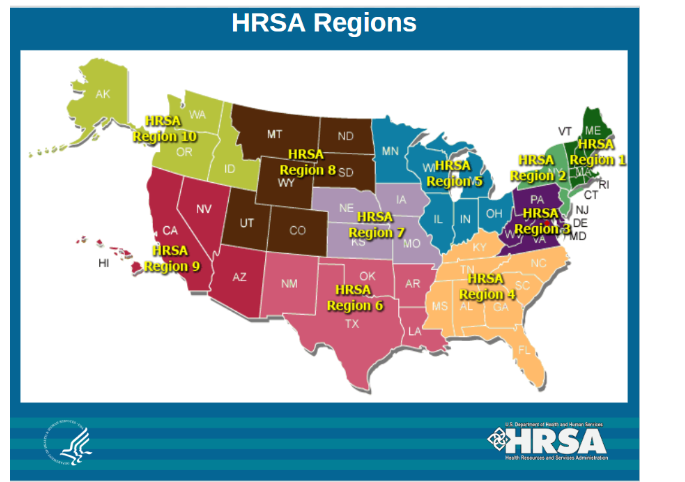
HRSA Regions
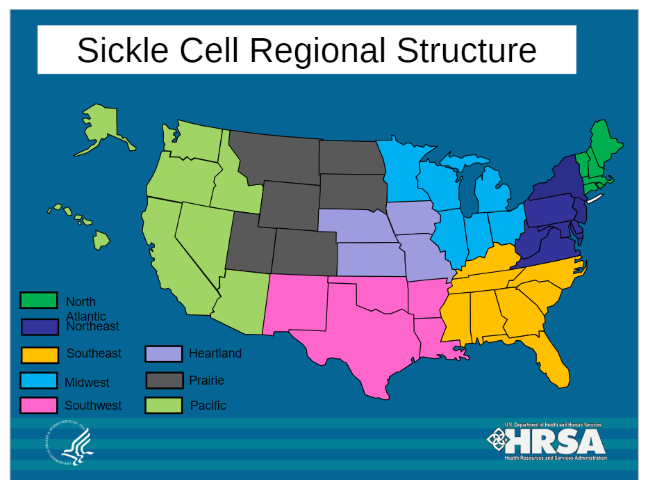
Sickle Cell Regional Structure
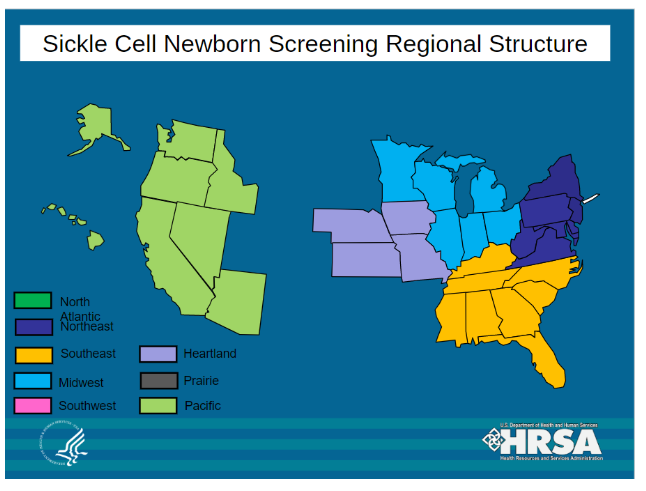
Sickle Cell Newborn Screening Regional Structure
1. Individuals living with sickle cell disease culturally refer to themselves as “Warriors” or “Sickle Cell Warriors”. | Coined in early 2000’s by nurse activist Tosin Ola in her original blog ‘Sickle Cell Can Kiss My @ss!
